Dry mouth, also known as xerostomia, is a common but often underestimated oral health issue. It can affect comfort, speech, chewing, swallowing, and long-term dental stability. If dryness continues, the risk of plaque, cavities, gum irritation, and oral infections can increase.
Quick Answer
Dry mouth usually has more than one cause. The most common are dehydration, medication side effects, chronic conditions, and lifestyle habits. The best approach is to identify the main trigger and combine hydration, preventive care, and case-specific professional support.

Causes of Dry Mouth
1. Dehydration
One of the most common causes is simple dehydration. When fluid intake drops, saliva production falls too. Even mild dehydration can cause sticky mouth sensation, bad breath, and speech discomfort. People who exercise heavily, consume high caffeine, or live in hot climates are more likely to notice this pattern.
Tip: target about 2 to 3 litres of water daily, and increase intake when consuming alcohol, coffee, or energy drinks.
2. Medications
More than 500 medications can list dry mouth as a side effect. Common groups include antidepressants, antihistamines, blood pressure drugs, and some pain medications. If dryness started after a medication change, discuss this with your physician before making any changes.
3. Systemic Medical Conditions
Some chronic conditions are strongly linked with xerostomia, including diabetes, Sjogren’s syndrome, neurologic conditions, and post-radiotherapy changes in head and neck patients. These situations usually need a combined medical and dental strategy.
4. Lifestyle Habits
- Smoking can reduce oral tissue circulation and worsen dryness.
- Frequent alcohol use can dehydrate oral tissues.
- High caffeine intake can worsen fluid loss for some patients.
- Mouth breathing during sleep can increase overnight dryness.
5. Age and Hormonal Changes
Dry mouth can become more common with age due to medication burden and physiologic gland changes. Hormonal shifts, including menopause, may also contribute in some patients.
How Can You Relieve Dry Mouth?
Relief depends on cause. Some patients improve quickly with hydration and habit changes. Others need long-term support and professional interventions.

1. Stay Hydrated
- Carry a water bottle and sip throughout the day.
- Set simple reminders if needed.
- Choose water over sugary drinks when possible.
2. Review Medications with Your Doctor
If symptoms started with a new prescription, your doctor may adjust dose, timing, or alternatives. Do not stop prescribed drugs on your own.
3. Use Saliva Substitutes and Alcohol-Free Mouthwashes
- Artificial saliva sprays and moisturising gels can improve comfort.
- Alcohol-free fluoride mouthwashes can help protect enamel.
4. Stimulate Saliva Production
- Chew sugar-free gum, ideally with xylitol.
- Use sugar-free lozenges.
- Include crunchy fibrous foods where clinically suitable.
5. Improve Daily Habits
- Reduce smoking, alcohol, and excessive caffeine.
- Use a bedroom humidifier if night dryness is frequent.

6. Maintain Strong Oral Hygiene
Low saliva increases plaque and decay risk, so consistency matters more than ever.
- Brush twice daily with fluoride toothpaste.
- Floss once daily.
- Consider an electric toothbrush for better plaque control.
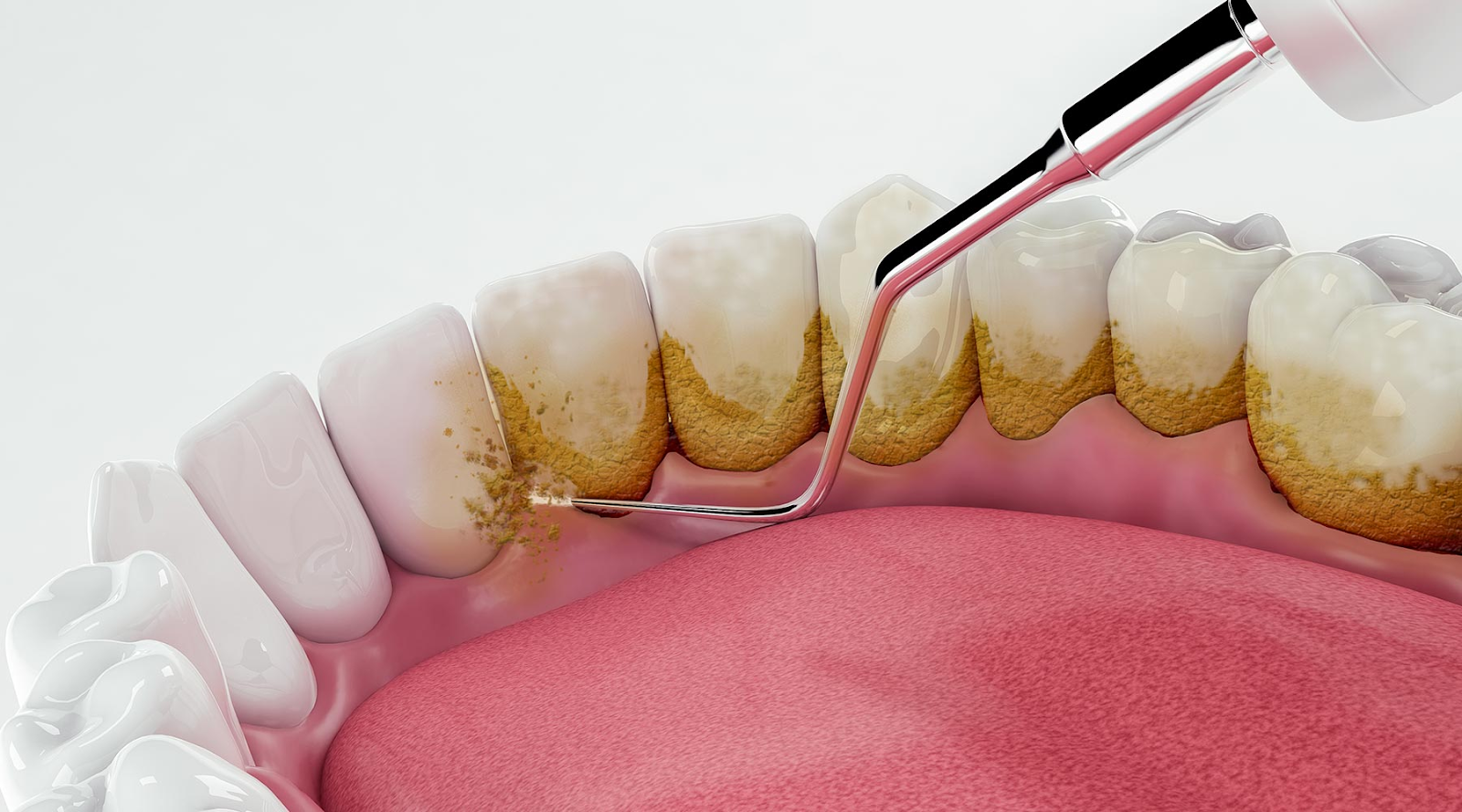
- Book regular professional cleaning visits.
7. Follow a Balanced Diet
Supportive nutrition can improve both oral and systemic resilience. Include vitamin C, vitamin D, omega-3 sources, and calcium-rich foods.
8. Professional Support for Persistent Cases
- Prescription saliva stimulants (case dependent).
- Custom fluoride trays for high-caries-risk patients.
- Closer recall intervals for prevention and monitoring.
9. Temporary Comfort Measures
- Keep water near your bed.
- Use ice chips for short-term moisture support.
- Avoid very salty or spicy foods when tissue irritation is high.
- Use lip balm to reduce cracked lips.
Lifestyle Adjustments That Make a Difference
Good dry mouth management is not only medical. Daily behavior changes often produce clear improvements within weeks.
- Reduce caffeine and alcohol where possible.
- Stop smoking or reduce significantly.
- Increase whole foods and hydration-focused routines.
- Use sugar-free xylitol gum to support saliva flow.
Advanced Treatments for Persistent Dry Mouth
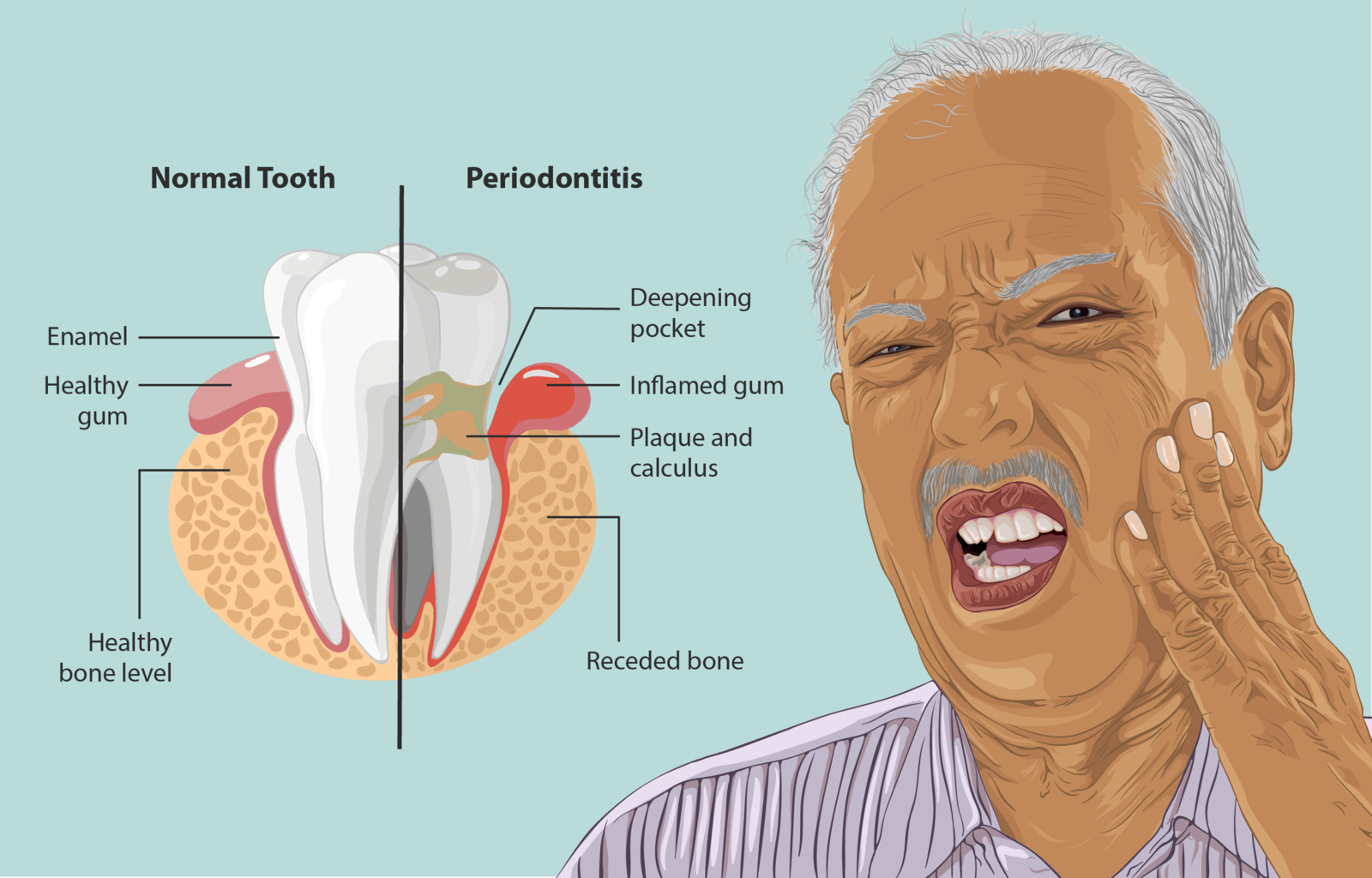
When dry mouth is linked to chronic conditions such as Sjogren’s syndrome or diabetes, hydration alone may not be enough. A structured medical-dental plan is usually required.
- Prescription medication where clinically indicated.
- Fluoride gels or mouthwashes for enamel protection.
- Moisturising sprays and gels to reduce tissue friction.
- Custom night appliances in selected severe cases.
Reference source: NHS guidance on Sjogren’s syndrome.
Complications of Ignoring Dry Mouth
Dry mouth is not only discomfort. If unmanaged, it may lead to secondary oral problems that become harder and more expensive to treat later.
| Complication | Explanation | Impact |
|---|---|---|
| Cavities | Less saliva means weaker natural cleansing and buffering. | More fillings, restorations, or crowns over time. |
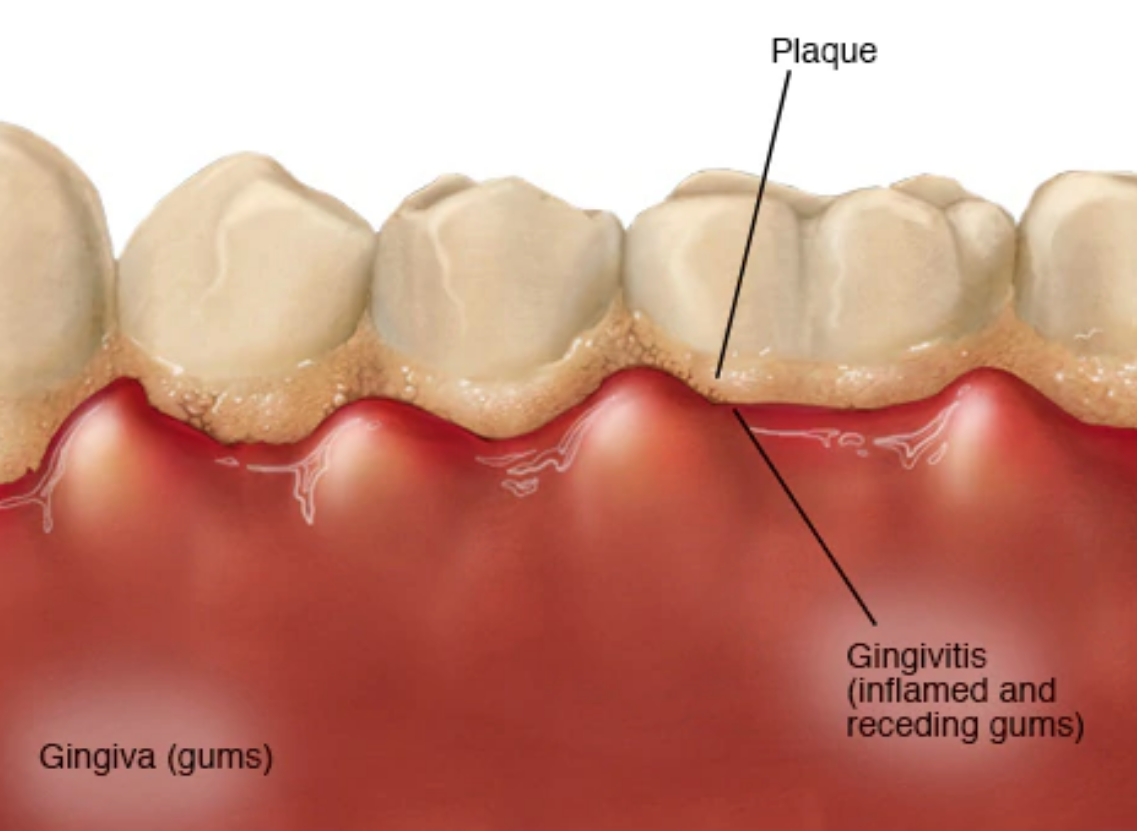
| Gum Disease | Bacteria can proliferate more easily in dry oral environments. | Bleeding, inflammation, and periodontal risk. |
| Oral Infections | Fungal infections like thrush are more common with low saliva. | Pain, patches, and eating discomfort. |
| Speech Difficulties | Dry tissues can interfere with articulation and comfort. | Social discomfort and reduced quality of life. |
When Should You See a Dentist?
Occasional dryness can be harmless. But persistent symptoms lasting more than two weeks should be assessed professionally.
- Persistent swallowing or speaking difficulty
- Burning tongue sensation
- Bad breath despite good hygiene
- Cracked lips, recurrent ulcers, or sore gums
- Denture fit changes due to dryness
Related reads: Plaque prevention guide and The role of saliva in oral health.
Frequently Asked Questions
Can dry mouth go away on its own?
Yes in temporary cases like short dehydration. Chronic cases usually need targeted management.
Is dry mouth dangerous?
It can become clinically significant if prolonged, especially due to increased decay and gum risk.
Do all mouthwashes help xerostomia?
No. Alcohol-containing mouthwashes can worsen dryness for some patients. Alcohol-free options are usually preferred.
Can implants or crowns be affected by dry mouth?
Yes. Reduced saliva can affect tissue comfort, plaque load, and long-term maintenance requirements.




