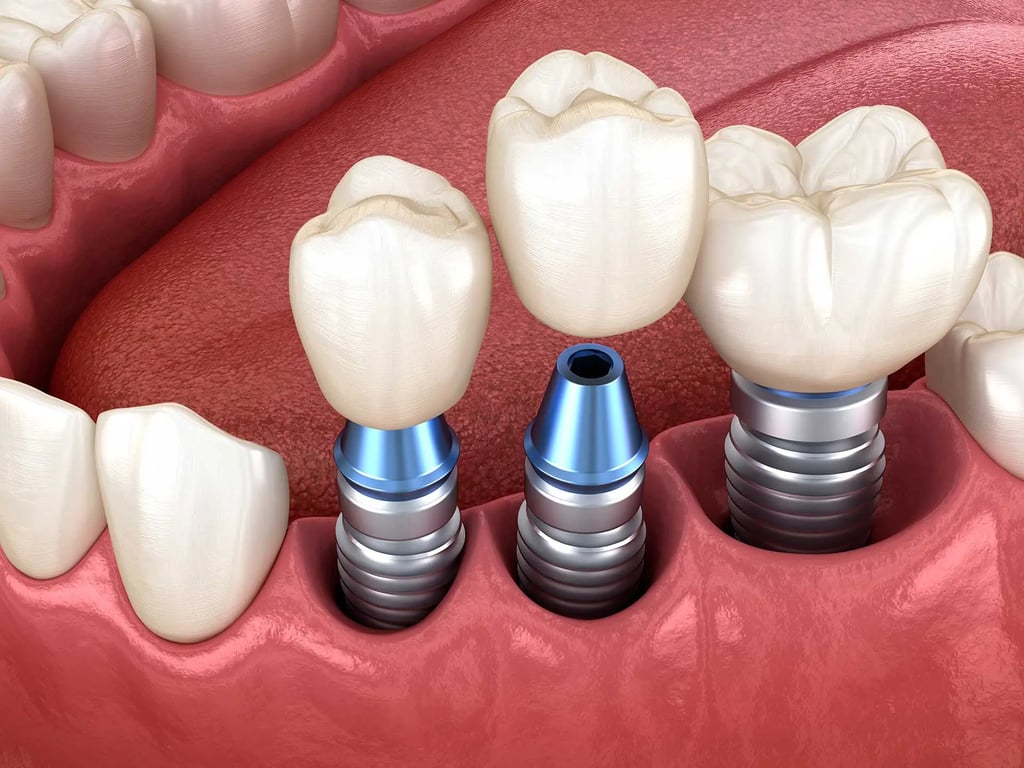
German Dental Implants in 2026: Complete Patient Guide
Losing a tooth is not only aesthetic. It can affect chewing, speech, bone support, and confidence. In 2026, many UK patients ask for German dental implants because they want strong engineering, long-term maintainability, and clear documentation. This guide explains what really matters before you commit.
Are German implants worth it in Turkey?
Short answer: yes, in the right hands. Brand quality helps, but diagnosis depth, surgical protocol, prosthetic design, and aftercare discipline decide real outcomes. A premium implant cannot fix poor planning.Entity and Keyword Map
Quick Answers
- Brand matters, but protocol matters more.
- German-origin systems are popular for engineering consistency and global serviceability.
- All-on-4 and All-on-6 are both valid; choice depends on anatomy and load profile.
- Written records and aftercare terms are essential before treatment starts.
- Best outcomes come from realistic planning and strict recall hygiene.
Why Implant System Choice Matters in 2026
Implant dentistry is no longer only “place and restore”. A successful outcome must be functional, cleanable, stable, and maintainable for years. Patients often compare only price per implant, but that misses the bigger clinical picture.
Long-term success depends on interconnected factors: gum baseline, bone anatomy, insertion stability, bite forces, parafunction control, and recall compliance. A good system supports this pathway, but it does not replace it.
Clinically, the strongest planning mindset is simple: choose a system that works not only on surgery day, but also on review years later.
What Makes German Implant Systems Distinctive?
There is no single “German formula”, but many German systems are known for manufacturing discipline, predictable component tolerances, and strong documentation ecosystems. For patients, this usually means clearer maintenance options and fewer surprises later.
- Consistent component fit and interface precision
- Mature material and surface-engineering pathways
- Broad prosthetic libraries for digital workflows
- Global distribution that supports future care continuity
These advantages are meaningful, especially in full-arch and high-load cases, where technical detail really matters.
Do Implant Brands Really Matter?
Yes, but never alone. A premium brand can support reliability and long-term serviceability. However, poor diagnosis or rushed surgery can still produce complications with any brand.
Where brand helps most
- Component availability and replacement access
- Large scientific evidence base
- Flexible restorative options for complex cases
Where protocol matters more than brand
- Ignoring active periodontal inflammation
- Immediate loading in unsuitable biology
- Weak occlusal planning in full-arch restorations
Top German Implant Brands in 2026
Straumann
Often selected for broad evidence depth, component ecosystem, and global service continuity. Commonly used in single and complex multi-unit cases.
Dentsply Sirona (Astra Tech)
Frequently preferred when soft-tissue stability and prosthetic contour precision are high priorities.
Nobel Biocare
Strong in digital and full-arch workflows, especially where staged prosthetic strategy is needed.
Zimmer Biomet
Used across routine and advanced indications, depending on anatomy, load conditions, and clinical strategy.
Dentaurum (tioLogic)
Often chosen in structured workflows that focus on long-term maintainability and practical restorative planning.
Materials, Surface Science, and Connection Design
Patients usually hear brand names first, but clinical behaviour comes from engineering details.
| Engineering dimension | Clinical relevance | Patient question |
|---|---|---|
| Alloy profile | Fatigue resistance under long-term load | Why this material for my case? |
| Surface properties | Early biologic response support | How does this affect loading timeline? |
| Connection architecture | Mechanical stability and serviceability | How will this be maintained in future? |
| Prosthetic ecosystem | Repair/replacement flexibility | Will parts be accessible in my country? |
Diagnostics and Treatment Planning Depth
Before discussing any implant brand, your clinician should complete full diagnosis: clinical exam, radiographic analysis, gum charting, bite review, and medical-risk screening.
In advanced cases, CBCT-guided planning is used to evaluate bone dimensions and anatomical safety zones. This improves positioning accuracy and can reduce avoidable risk.
Single Implant vs Full-Arch Pathways
Single-tooth replacement and full-arch reconstruction are not the same treatment logic.
Single implant priorities
- Precise 3D positioning and emergence profile control
- Soft-tissue harmony in aesthetic zones
- Natural bite integration with adjacent teeth
Full-arch priorities
- Cross-arch force distribution and framework stability
- Hygiene-accessible prosthetic contours
- Structured transition from provisional to definitive restoration
All-on-4 vs All-on-6
Both concepts are valid in the right case. The decision should follow anatomy, force profile, and clinician strategy.
| Dimension | All-on-4 | All-on-6 |
|---|---|---|
| Implants per arch | 4 | 6 |
| Load distribution | Higher load per implant | More distributed load profile |
| Typical indication logic | Can be efficient in selected reduced-bone anatomy | Often selected for added structural redundancy |
| Decision driver | Stability + anatomy + prosthetic plan | Stability + anatomy + prosthetic plan |
Related internal guides: All-on-4 vs All-on-6 in Turkey and Dental Implants in Turkey.
Surgery Quality and Immediate Loading Rules
Great outcomes need controlled surgical execution: sterile protocol, atraumatic handling, objective stability checks, and clear post-op instructions.
- Pre-op checklist and hygiene protocol
- Precision placement according to prosthetic goals
- Objective primary-stability criteria
- Documented loading decision, not marketing pressure
Prosthetic Design and Long-Term Maintainability
Implant surgery is only half of the story. Final prosthetic design determines daily comfort, cleanability, and technical durability.
- Passive fit to reduce mechanical stress
- Balanced occlusion for load control
- Contours that allow practical hygiene access
- Material strategy based on function and serviceability
In many advanced pathways, provisional restorations are used as functional prototypes before final delivery.
Cost vs Value: How to Compare Fairly
Two quotes can look similar but include very different scope. Compare complete pathway value, not just implant unit price.
- Diagnostics and imaging depth
- Surgical staging and provisional phase inclusion
- Definitive prosthetic design and adjustment policy
- Documentation package and aftercare terms
- Complication management route
Explore more: German implant brands and prices guide.
Risks and Mitigation Strategy
Biological risk areas
- Delayed integration
- Peri-implant soft-tissue inflammation
- Healing disruption from systemic factors
Technical risk areas
- Component or screw issues
- Prosthetic chipping/fracture under heavy load
- Framework stress from poor occlusal design
Main risk drivers
- Untreated gum disease
- Smoking and poorly controlled diabetes
- Bruxism without protective planning
- Missed maintenance recalls
Patient Checklist Before You Commit
- Is diagnosis complete and documented?
- Is the treatment timeline biological, not sales-driven?
- Are implant and prosthetic components specified in writing?
- Is immediate loading decision explained with objective criteria?
- Are aftercare intervals and escalation pathways clear?
- Will you receive full records for future follow-up in the UK?
Frequently Asked Questions
Are German implant systems always the best option?
Not in every case. They are often excellent options, but final selection depends on anatomy, function, and treatment goals.
Does premium brand guarantee success?
No. Success needs correct diagnosis, skilled execution, stable prosthetics, and maintenance compliance.
Can I be suitable for immediate loading?
Possibly. Suitability is decided after clinical diagnostics and objective stability assessment.
Will my local dentist be able to maintain treatment later?
Often yes, especially if you keep full implant and prosthetic documentation.
How much does smoking affect implant outcomes?
Quite a lot. Smoking raises healing and long-term tissue complication risk.
How long do implant restorations last?
It varies by case, loading profile, and maintenance. Think of implants as a lifelong care pathway, not a one-time fix.


