Имплантация зубов All-on-4 против All-on-6 в Турции: Что подойдет именно вам? (Путеводитель по Великобритании 2026)
A practical, evidence-aware comparison for UK patients considering full-arch implant treatment in Antalya. This revised guide explains what truly separates All-on-4 from All-on-6, who usually fits each route, when immediate teeth are realistic, and how to compare clinics on planning quality rather than marketing language.
Clinical review: Дт. Фуркан Озтюрк и Dt. Zübeyde Özlem Zeren на Центр улыбок Турция.
How this guide was prepared: It follows prosthetic-led full-arch planning principles used for international patients at Smile Center Turkey, alongside public guidance on implant maintenance, peri-implant risk management, staged treatment pathways, and UK patient travel planning. Final suitability always depends on in-person examination, CBCT imaging, periodontal status, bite analysis, and medical history.
Quick Answer
Neither option is automatically “better”. Все на 4 is often chosen when posterior bone is limited and graft-minimisation matters. Все на 6 is often preferred when anatomy allows two additional implants and the goal is broader load sharing under function. In practice, the right choice depends on bone volume, implant stability, bite force, parafunction risk, bridge design, hygiene access, and how predictable the long-term maintenance plan is.
Введение
All-on-4 and All-on-6 are both full-arch implant concepts used to restore a complete upper or lower jaw with a fixed bridge supported by implants. The visible difference is implant count. The clinically important difference is how implant number, position, angulation, and prosthetic design work together to manage force, hygiene, and long-term maintenance.
For UK patients, the practical question is not which label sounds stronger. It is which protocol best matches anatomy, bite profile, treatment tolerance, and post-return follow-up. The best plan is the one that is biologically sensible, prosthetically cleanable, and realistic to maintain once you are back home.
1. What Full-Arch Dental Implants Actually Are
Full-arch implant rehabilitation replaces all teeth in one jaw using a fixed bridge attached to implants. Compared with removable dentures, fixed full-arch prostheses can improve stability, chewing confidence, speech control, and day-to-day comfort. They are, however, complex surgical-restorative treatments rather than one-day cosmetic purchases.
- Фиксированный мост: usually screw-retained so it can be reviewed and serviced when needed.
- Немедленный временный вариант: possible in selected cases if implant stability and bite control are adequate.
- Definitive bridge: usually delivered after healing and functional validation.
- Lifelong review: peri-implant tissues and prosthetic components need regular monitoring.
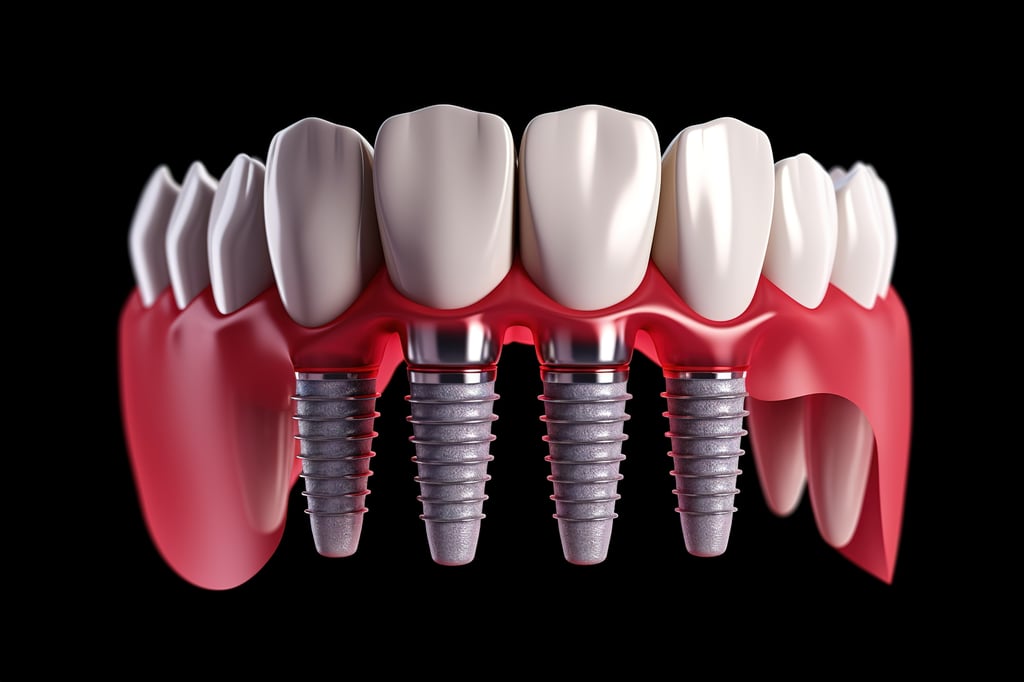
2. All-on-4: Where It Tends to Fit
All-on-4 uses four implants to support one full-arch bridge. In many protocols, the two front implants are more upright and the posterior implants are angled to use available bone and limit distal cantilever length.
Потенциальные сильные стороны
- Can be useful when posterior bone is limited and graft-minimisation is a planning priority.
- Lower implant count may simplify surgery in selected cases.
- Strategic angulation can help avoid some anatomical limitations in the posterior jaw.
- Well-established option for selected edentulous or failing-dentition cases.
Чувствительность к планированию
- With fewer support points, bridge design and cantilever control become more important.
- High bite force and bruxism require tighter occlusal management.
- Implant positioning tolerance is smaller when the prosthesis depends on only four fixtures.
- Hygiene access and prosthetic emergence must still be protected; speed should not override cleanability.
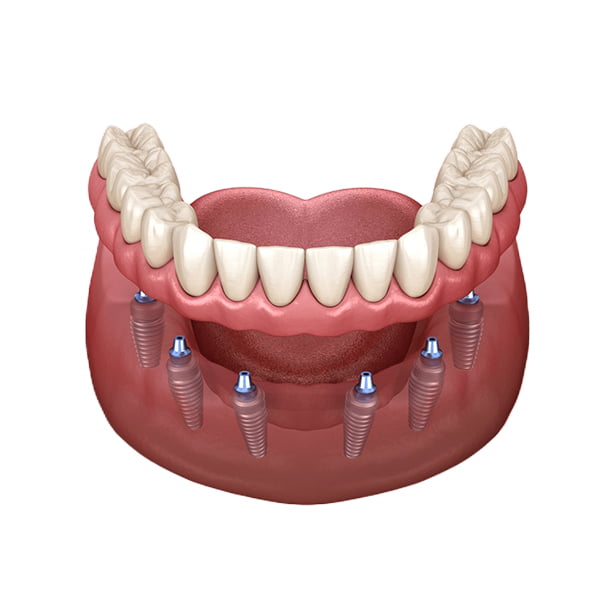
3. All-on-6: Where It Tends to Fit
All-on-6 uses six implants to support the arch. The two additional support points can broaden load distribution and may provide more restorative flexibility when bone quality, arch form, and implant spacing allow.
Потенциальные сильные стороны
- More support points can improve force sharing across the bridge.
- Often attractive in patients with stronger bite patterns or higher functional demand.
- May reduce stress per implant and allow greater restorative redundancy in suitable cases.
- Can be favourable where bone volume and implant spacing are sufficient for six stable fixtures.
Чувствительность к планированию
- Usually requires anatomy that comfortably accommodates six well-positioned implants.
- May increase surgical scope and chair-time.
- More implants do not correct poor bridge design, poor hygiene access, or unmanaged parafunction.
- Additional fixtures only help if they are placed in restoratively useful positions.
4. All-on-4 против All-on-6: Краткое сравнение
| Фактор | Все на 4 | Все на 6 |
|---|---|---|
| Количество имплантатов | 4 implants per arch | 6 implants per arch |
| Типичный приоритет планирования | Strategic support with graft-minimisation in selected anatomy | Broader support distribution where bone allows |
| Потребность в костях | Can be more forgiving in some posterior-bone-limited cases | Usually needs sufficient anatomy for six useful implant positions |
| Load sharing | Good in appropriate cases with tight bridge design | Can offer wider distribution potential |
| Surgical scope | Часто короче | Often broader and slightly longer |
| Immediate provisional sensitivity | Highly dependent on primary stability and occlusal control | Also dependent on stability; extra support points may help in selected cases |
| Often considered for | Selected atrophic or graft-avoidance cases | Higher functional demand when anatomy allows |
| Main trade-off | Less redundancy if one implant or support zone is compromised | More surgery and not automatically better if positions are poor |
5. Evidence Snapshot: What Current Studies Suggest
Current evidence does not support a blanket statement that one approach is always superior. Recent comparative research suggests that both four-implant and six-implant full-arch concepts can perform predictably when anatomy, loading strategy, and prosthetic design are appropriate.
6. Biomechanics and Load Control
Biomechanics sits at the centre of full-arch success. Chewing force is transmitted from the bridge through the implants into bone. Implant number is only one part of the system. Stress behaviour is also affected by arch shape, anterior-posterior spread, cantilever length, implant angulation, implant diameter, opposing dentition, parafunction, framework stiffness, and occlusal design.
In simple terms, more support points may reduce the force concentration carried by each implant. But a poorly designed All-on-6 bridge can still overload. Likewise, a well-planned All-on-4 can perform very predictably when the case is selected properly and the bridge is disciplined in its design.
- Cantilever control: one of the most important determinants of long-term stress behaviour.
- Parafunction: clenching or bruxism changes the risk profile and may influence implant number, material choice, and nightguard planning.
- Opposing bite: a fixed arch opposing natural teeth or another fixed arch behaves differently from an arch opposing a denture.
- Bridge rigidity: framework design and restorative material alter how force is transferred across the arch.
7. Who Is a Candidate — and Who Should Pause
Good candidate selection starts with diagnosis, not price. CBCT imaging, periodontal assessment, medical history, and bite evaluation should all be part of planning before a full-arch recommendation is finalised.
8. Digital Planning and Guided Surgery
Modern full-arch workflows commonly combine CBCT with intraoral scans and virtual prosthetic planning. This allows the team to plan implant positions against the final bridge rather than placing implants first and “making the teeth fit later”.
9. Bone Grafting, Sinus Lift and Staged Cases
One reason All-on-4 became so popular is that posterior angulation can sometimes reduce the need for grafting. That does not mean grafting is never required. Severe bone loss, sinus anatomy, arch form, or soft-tissue deficiencies may still justify sinus lift procedures, grafting, short-implant strategies, or an alternative full-arch protocol.
The correct question is not “Can this be done without grafting at all costs?” It is “What approach gives the safest long-term foundation for this bridge?” In some very resorbed upper jaws, the safer pathway may be staged reconstruction or a different advanced solution entirely.
- Posterior maxillary deficiency may raise sinus-lift considerations.
- Severe ridge resorption can influence implant angulation, implant length, and prosthetic space.
- Very advanced atrophy may require treatment concepts beyond conventional All-on-4 or All-on-6.
- A graft-free plan is only a virtue when it is also a sound biological plan.
10. Bridge Materials and Design Choices
Definitive full-arch bridges are not all made the same way. Material selection should follow occlusion, arch space, aesthetic goals, reparability needs, and the maintenance burden the patient can realistically manage.
| Material / Design | Typical Role | Main Practical Point |
|---|---|---|
| PMMA / acrylic provisional | Healing and adaptation phase | Useful while tissues settle and occlusion is refined; not the same as the definitive bridge. |
| Monolithic zirconia | Definitive bridge option | Strong and wear-resistant, but still needs careful occlusal design and maintenance discipline. |
| Zirconia over titanium or titanium-supported bridge | Definitive long-span support option | Can be attractive where rigidity, passive fit, or long-span support are key planning concerns. |
| Hybrid approaches | Case-specific compromise | No single material is best for every full-arch case; design logic matters more than prestige wording. |
11. Treatment Timeline for UK Patients
Many full-arch cases are two-visit pathways rather than “finish everything once and forget it”. Immediate provisional teeth may be placed on the first visit if the case qualifies, but the definitive bridge is usually delivered after healing and reassessment.
- Удаленная сортировка: medical history, photos, scans if available, and initial planning discussion.
- Поездка 1: diagnostics, extractions if required, implant surgery, and provisional bridge only if stability and bite criteria are met.
- Healing phase: controlled loading, tissue adaptation, review of comfort, speech, hygiene, and function.
- Поездка 2: definitive bridge records, try-in, fit, torque protocol, and occlusal refinement.
- Post-return continuity: implant-specific maintenance and a clear record pack for future clinicians.
12. What to Confirm in Writing Before Booking
Headline pricing does not tell you whether two quotes are genuinely comparable. The meaningful comparison is treatment scope, implant system, prosthetic phase, exclusions, and how complications or adjustments are handled after you fly home.
- Diagnostics: Is the plan CBCT-led and prosthetic-led, or only based on a panoramic view and a package template?
- Implant system: Brand, component traceability, and whether records will be provided to you.
- Loading logic: Is an immediate provisional included, and what clinical criteria determine whether it is safe?
- Definitive bridge: Material, retention method, timeframe, and what is included in the final phase.
- Exclusions: Bone grafting, sinus lift, sedation, medications, extractions, repairs, and re-fits.
- Revision policy: What happens if adjustments are needed after you return to the UK?
- Пакет документации: Implant details, component references, imaging, and post-op instructions.
- Communication: Named treating clinicians and a clear escalation route for urgent concerns.
13. Risks, Maintenance and Longevity
Complications in full-arch treatment are usually biological, mechanical, or logistical. The strongest protection is disciplined planning, careful loading decisions, and long-term maintenance rather than aggressive same-day marketing.
What long-term maintenance usually involves
- Implant-specific supportive care rather than generic routine cleaning alone.
- Risk-based recall intervals set according to periodontal and peri-implant status.
- Daily bridge cleaning with the tools advised for the prosthesis design.
- Nightguard use where bruxism or clenching increases overload risk.
- Periodic review of occlusion, screw-retained components, and soft-tissue health.
14. FAQs
Is All-on-6 always stronger than All-on-4?
Can All-on-4 later be converted to All-on-6?
Всегда ли мне нужна костная пластика?
Can I leave Antalya with fixed teeth on my first trip?
Will UK dentists maintain implants placed abroad?
15. References
- Scottish Dental Clinical Effectiveness Programme (SDCEP) — General care of dental implants
- SDCEP — Managing peri-implant disease risk
- Royal College of Surgeons of England, Faculty of Dental Surgery — Guidance on the standards of care for NHS-funded dental implant treatment (2019)
- European Association for Osseointegration (EAO) — consensus summary on timing of loading
- Academy of Osseointegration / American Academy of Periodontology — consensus on prevention and management of peri-implant diseases
- Zhang Y, et al. Comparison of 4- or 6-implant supported immediate full-arch fixed prostheses: retrospective cohort study (2023)
- Caramês JMM, et al. Four vs. Six Implant Full-Arch Restorations — direct comparative retrospective analysis (2025)
- Soto-Peñaloza D, et al. The All-on-Four treatment concept: systematic review
- Werny JG, et al. Freehand vs. computer-aided implant surgery: systematic review and meta-analysis (2025)
- General Dental Council — Going abroad for dental treatment
- NHS — Treatment abroad checklist
Educational content for patient awareness only. It is not a diagnosis or a substitute for clinical examination, informed consent, or individual treatment planning.
Ready for a Case-Based Full-Arch Plan?
The most useful next step is not choosing a slogan. It is getting a written plan based on imaging, periodontal status, bite risk, and a realistic timeline for provisional and final teeth.
Structured planning • Written scope • Diagnosis before promises
Счастливые истории
Very happy with my treatment at Smile Center Turkey
Very happy with my treatment at Smile Center Turkey. Staff are friendly and professional and there's a comfortable atmosphere, with a lovely garden to spend time in before and after treatment, which is a little oasis in…
Это, безусловно, лучший стоматолог в Турции,
Это, безусловно, лучший стоматолог в Турции, заботливые, сострадательные, заслуживающие доверия люди, которые не могут сделать достаточно, чтобы помочь вам. Полностью заслуживают доверия и действительно убеждаются, что вы очень довольны, прежде чем уйти. Они не будут не...
С самого первого контакта с центром "Смайл",
С самого первого контакта с Smile Center все было профессионально, гладко и легко. Общение было фантастическим, и на все вопросы я получал своевременные ответы. В день процедуры я чувствовал себя спокойно...
Замечательные люди и великолепная клиника! Я должен сказать.
Величайшие люди и величайшая клиника! Я должна сказать, что это место просто потрясающее! От самого счастливого и дружелюбного персонала до быстрых, профессиональных и безболезненных процедур, мгновенных и подробных ответов, когда я...
⭐️⭐️⭐️⭐️⭐️ Я не могу порекомендовать Smile Centre Turkey достаточно высоко.
⭐️⭐️⭐️⭐️⭐️ Я не могу рекомендовать Smile Centre Turkey достаточно высоко. Начиная с самой первой консультации и заканчивая окончательной установкой коронок и имплантатов, уровень заботы, профессионализма и внимания к деталям был о...


