Dental implants are one of the most reliable long-term ways to replace missing teeth, but they are not a “fit it and forget it” treatment. If you are asking how long implants last, the honest answer is this: many can stay in function for well over a decade, some for 20 years or more, but longevity depends on planning, bone and gum health, plaque control, smoking, grinding habits, and regular professional review. This guide explains what really protects implant lifespan — and what tends to shorten it.
How this guide was prepared: It combines current long-term implant survival data, UK implant-maintenance guidance, and the practical implant aftercare principles used for international patients in Antalya. It is educational and does not replace an in-person examination.
Short Answer
Well-planned dental implants can last a very long time, but no honest clinic should promise the same lifespan for every patient. The implant fixture in the bone may outlast the crown, bridge, screw or gum condition around it. In practical terms, long-term success depends less on one surgery day and more on what happens afterwards: cleaning, monitoring, bite control, smoking avoidance, and early management of inflammation.
Entity and Search Intent Map
Patients often search different phrases for the same real-world concern:
Most implant problems are not dramatic day-one failures. They are slow issues in hygiene, inflammation, overload, or follow-up.
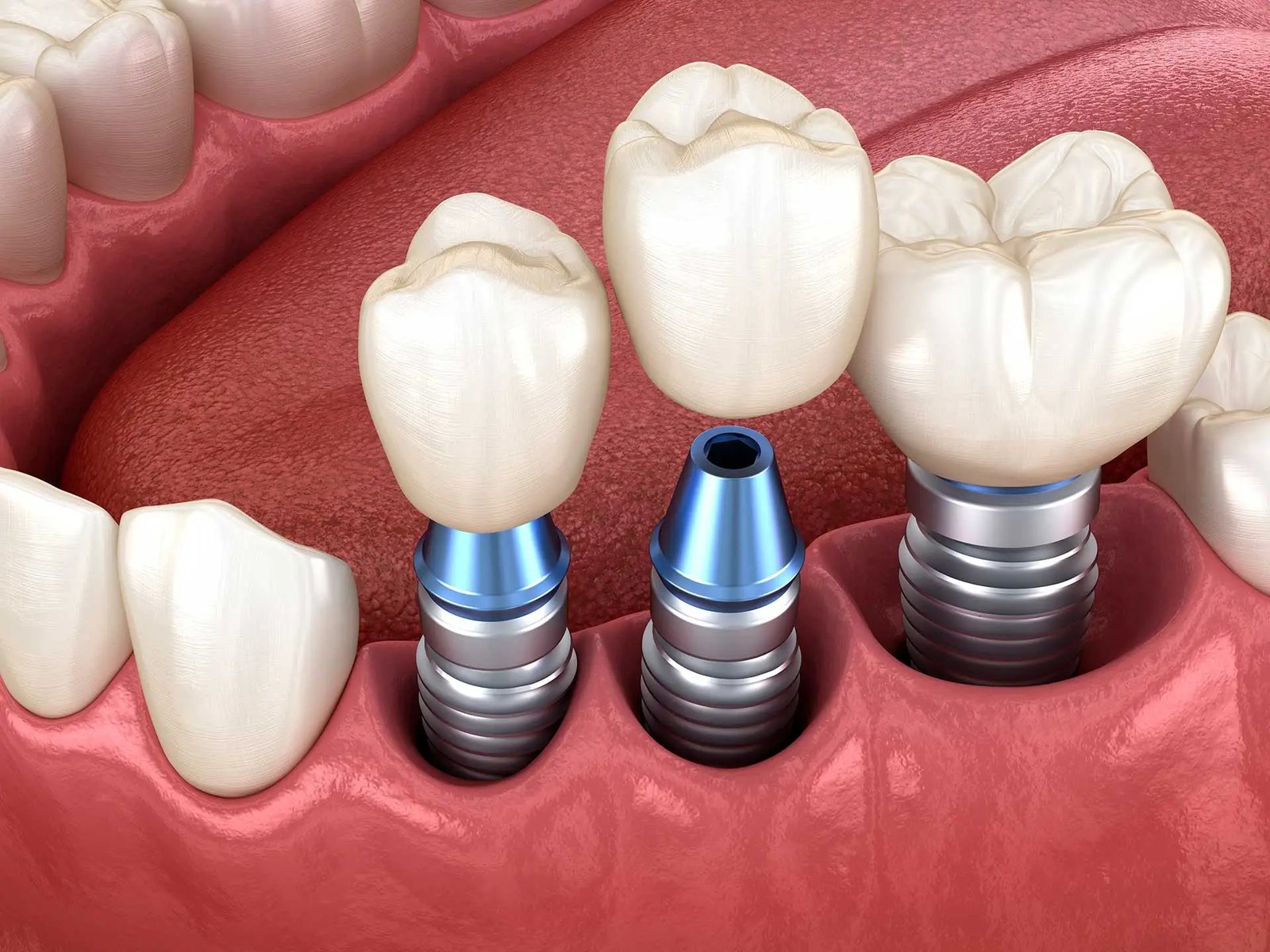
1. How Long Implants Last in Real Life
Patients usually want one neat number. Dentistry does not work quite like that. Implant lifespan is better understood in layers: the implant fixture in the jawbone, the abutment or screw connection, and the visible crown or bridge. These do not all age at the same speed.
The broad long-term evidence is encouraging. A 2019 systematic review reported a 10-year implant-level survival estimate of 96.4%. A newer 20-year meta-analysis suggests that roughly four out of five implants remain in function at that point. That is strong performance by medical standards — but it is not a promise for every mouth.
Some implants last decades without major trouble. Others fail earlier because the biology was difficult from the outset, the patient had unstable gum disease, smoking continued, plaque control was poor, or excessive bite force was not managed properly. The safest way to explain longevity is this: implants can last a long time, but they are not maintenance-free and they are not immune to disease.
2. Implant Fixture vs Crown: What Usually Needs Work First?
When patients say “my implant failed”, they often mean something different. Sometimes the implant fixture has genuinely lost integration. But quite often the issue is the crown, the bite, soft tissue inflammation, a loose screw, or plaque retention around the restoration.
| Part of the treatment | What it does | What tends to happen over time | What helps it last |
|---|---|---|---|
| Implant fixture | Titanium or similar implant anchored in bone | Can remain stable for many years if integration and tissue health are maintained | Good planning, healthy gums, smoking control, regular monitoring |
| Abutment / screw components | Join the implant to the visible restoration | Can loosen or need servicing, especially under overload | Accurate bite adjustment, night guard where needed, component traceability |
| Crown or bridge | Visible tooth replacement above the gumline | May chip, wear, stain, or need replacement before the fixture does | Material choice, hygiene, avoiding destructive habits, periodic review |
| Gums and surrounding bone | Support the implant biologically | Can become inflamed or lose bone if plaque control slips | Daily cleaning, supportive peri-implant care, early treatment of bleeding |
This distinction matters because it changes the tone of the conversation. A loose crown is not the same as a failed implant. Bleeding gums around an implant do not automatically mean the fixture is lost. But both still deserve prompt review because early intervention is usually easier and cheaper than late rescue.
3. Daily Home Care That Matters Most
The long-term success of implant treatment depends heavily on what you do when you are back at home. Plaque is still plaque. Implants do not get tooth decay, but the tissues around them can still become inflamed, and peri-implantitis is one of the most important causes of implant problems over time.
Brush properly, not aggressively
Brush twice daily using a soft brush or an electric brush head that your dentist is happy with. The aim is to clean around the gum margin without scrubbing the tissues raw. Heavy-handed brushing is not “better cleaning”. It can simply make a sore mouth sorer.
Clean between the teeth or around the bridge every day
This is where many patients struggle. The right tool depends on the design:
- Single implant crown: floss, superfloss, floss threaders or small interdental brushes may all help.
- Implant bridge: you may need threaders, interdental brushes, or a water flosser to reach under the pontic area.
- Full-arch fixed bridge: cleaning is more technique-sensitive and should be demonstrated properly before you leave the clinic.
Do not rely on mouthwash alone
Mouthwash can be useful in specific situations, but it does not replace brushing and mechanical plaque removal. Short courses of chlorhexidine or other prescribed rinses are sometimes used after surgery or around inflamed tissues, but they are an adjunct, not the main treatment.
4. Food, Hydration and Everyday Habits
Diet affects implant longevity in a practical way rather than a glamorous one. In the early healing phase, your own surgeon may recommend a soft-food period, especially after surgery or grafting. Later on, once the implant is integrated and the final crown is fitted, you can usually eat normally. But “normal” does not mean using your restorations as tools.
- Avoid chewing ice, cracking nutshells, or biting very hard sweets.
- Be cautious with sticky foods if you have provisionals, large bridges, or extensive restorative work.
- Do not open packaging with your teeth.
- Stay well hydrated to support saliva flow and comfort.
- Keep sugary snacking frequency low, especially if you also have natural teeth and gum disease risk.
Good hydration is more relevant than many people realise. Saliva is one of the mouth’s main protective systems. It helps buffer acids, dilute bacteria, improve comfort, and reduce the sticky mouth feeling that makes plaque control harder. If you are prone to dry mouth, saliva support becomes part of implant protection too.
5. Sports, Grinding and Overload Protection
Many implant complications are not caused by infection alone. Some are mechanical. If you clench or grind your teeth, or if you play contact sport, your restorations may be exposed to repeated excessive force.
Night guards matter if you grind
Bruxism does not automatically rule out implants, but it does increase the risk of mechanical problems. UK hospital guidance warns that grinding habits can overload implants and reduce success rates. A custom night guard can help protect crowns, screws, ceramics and surrounding tissues, especially in patients who wake with tight jaw muscles or headaches.
Mouthguards matter if you play sport
If you box, play rugby, hockey, martial arts, or any contact sport, use a proper mouthguard. Implant crowns do not have the same shock-absorbing periodontal ligament that natural teeth do, so trauma protection matters.
Stress management is not irrelevant
Not all grinding is stress-related, but stress and anxiety can worsen clenching in many people. Better sleep, lower stress load, and awareness of daytime clenching can all help protect implant-supported work.
6. Professional Maintenance and Follow-Up
Implants need professional review just like natural teeth do. In current peri-implant maintenance guidance, the strongest long-term outcomes are linked to structured supportive care rather than one-off treatment followed by neglect. In practical terms, that means regular checks of plaque levels, bleeding, pockets, bone stability, bite, and restoration fit.
High-risk patients are often reviewed more frequently. After treatment for peri-implant disease, intervals may initially be as close as three or four months. For stable low-risk patients, maintenance may later settle into longer personalised intervals. The point is not a one-size-fits-all number; the point is that irregular follow-up is a known risk factor for biological complications and implant loss.
If you had implants abroad, records are essential
Before you fly home, ask for:
- implant system and component references
- baseline radiographs or imaging summary
- restoration type and material notes
- aftercare instructions and review schedule
- urgent contact route if you are worried later
That record pack makes local follow-up much easier for any UK dentist or hygienist who needs to maintain the case.
7. Smoking, Diabetes and Gum History
Some implant risks are modifiable, and these are the ones worth taking seriously before you spend money on treatment.
Курение и вейпинг
Smoking impairs wound healing and is consistently associated with higher complication and failure rates. UK implant guidance is unusually firm on this point. That does not mean every smoker will lose every implant, but it does mean the odds are worse — especially if hygiene and gum health are already weak.
Poorly controlled diabetes
Implants and diabetes can work together, but glycaemic control matters. When blood glucose is poorly controlled, wound healing and infection resistance are less predictable. Stable control is the safer route, and it should be part of treatment planning rather than an afterthought.
Previous periodontitis
If you have lost teeth because of gum disease, you are not automatically excluded from implants. But you do move into a higher-risk category. Current guidance shows that patients with a history of periodontitis have a higher risk of peri-implant disease unless the condition is stabilised and maintained properly.
8. What Is Normal After Surgery and What Needs Review?
A lot of anxiety about implant survival comes from not knowing what is normal in the first week. Some soreness and swelling are expected. That alone does not mean failure.
| Likely normal early healing | Needs review sooner rather than later |
|---|---|
| Mild to moderate soreness for the first few days | Pain that is getting worse instead of better after day 3 |
| Swelling that peaks around 48 to 72 hours | Increasing swelling, fever, discharge, or a persistent bad taste |
| Tenderness when cleaning the area gently | Bleeding, suppuration or a loose-feeling implant |
| Gradual improvement over the first week | A site that feels non-healing after the expected early window |
A loose healing cap or loose crown is not identical to implant failure, but it still needs attention. The important rule is simple: mobility of the implant fixture itself is never normal.
9. How Implants Work, Briefly
A dental implant replaces the root of the missing tooth with a small titanium or titanium-alloy fixture placed in the jawbone. During the healing period, bone attaches to the implant surface. This biological bond is called остеоинтеграция.
After that healing phase, the implant is restored with a crown, bridge, or full-arch prosthesis depending on the case. In many straightforward cases, osseointegration takes around three to six months, but the timing varies according to bone quality, loading strategy, grafting, medical factors, and overall case complexity.
10. How to Choose a Reliable Implant Clinic
Implant longevity starts before surgery. It starts with clinic choice. If you are considering treatment abroad, including in Turkey, compare clinics on process quality, not just the first quote.
- Ask for diagnostics: CBCT planning, gum assessment, bite analysis, not just a WhatsApp package quote.
- Ask which implant system will be used: brand and component traceability matter later.
- Ask who is treating you: named clinicians, not generic “our team”.
- Ask about aftercare: what happens if you are back in the UK and need advice?
- Ask for real cases: before-and-after examples relevant to your problem, not only the most dramatic marketing shots.
- Ask for written scope: what is included, what is staged, and what may change after full diagnosis.
At Smile Center Turkey, the live implant price list currently shows Osstem from £400 and Megagen AnyRidge from £450 per implant, with prices listed in GBP for UK and international patients. That is useful for transparency — but price still needs to be matched against implant brand, component set, diagnostics, grafting needs, and follow-up structure.
Часто задаваемые вопросы
Can dental implants last a lifetime?
Some do, but that should not be sold as a universal promise. A more realistic answer is that many implants function for a very long time when diagnosis, hygiene, gum stability and maintenance all stay favourable.
What usually needs replacing first — the implant or the crown?
Quite often it is the crown, the bridgework, or a screw-related component rather than the fixture in the bone. Soft-tissue inflammation can also create problems before the implant itself is lost.
Do I need special cleaning tools around implants?
Usually yes, but the right tool depends on the restoration. A single implant crown is cleaned differently from a fixed bridge or a full-arch prosthesis. Your implant team should demonstrate the exact technique.
Can smoking really shorten implant life?
Yes. Smoking is one of the clearest modifiable risk factors for healing complications, tissue inflammation and implant failure. Reducing or ideally stopping before treatment improves the odds.
How often should implants be checked?
There is no single interval for everyone. Many patients are monitored every three to six months initially or if they are high risk, then moved to a tailored schedule once the case is stable.
Can a UK dentist maintain implants placed in Turkey?
In many cases yes, especially if you return with clear records, implant system details, component references and baseline radiographs.
Ссылки
- Howe MS, Keys W, Richards D. Long-term (10-year) dental implant survival: a systematic review and sensitivity meta-analysis.
- Kupka JR et al. A 20-year meta-analysis of dental implant survival rates.
- Perussolo J et al. Maintenance of peri-implant health in general dental practice.
- UK Government / Delivering Better Oral Health: peri-implantitis overview.
- Cambridge University Hospitals: Dental implants in restorative dentistry.
- Royal College of Surgeons of England: Guidance on standards of care for dental implant treatment.
- Guy’s and St Thomas’ NHS Foundation Trust: After having a dental implant.
- NHS: Teeth grinding (bruxism).
Похожие гиды
Want a Case-Based Implant Assessment?
Share your X-rays, photos and main concerns with the Smile Center Turkey team. You can receive a no-obligation review, a realistic staged plan, and a clearer idea of what your case may involve before you commit.
Structured planning • UK-friendly coordination • Diagnosis before promises


